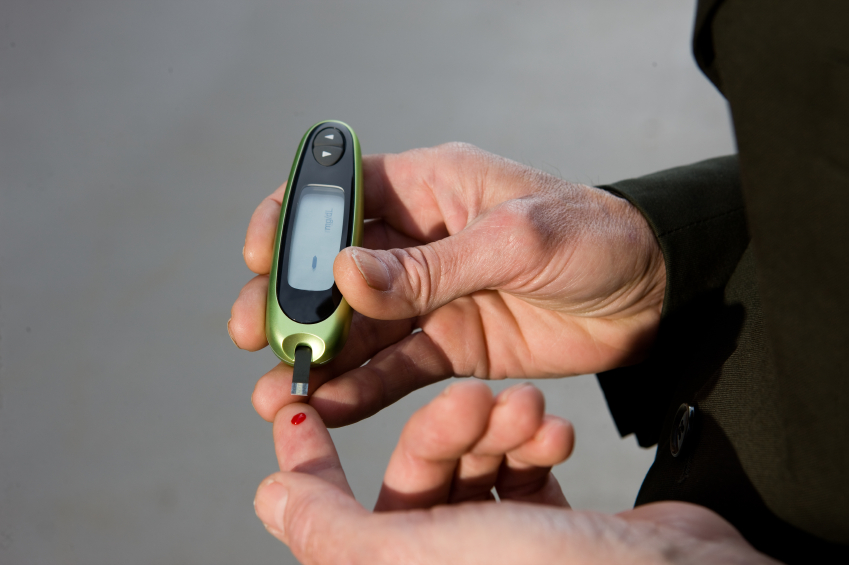
Look to your feet for the first signs of diabetes
08/21/2018 / By Russel Davis
Thorough foot assessment may prove effective in identifying patients at risk of developing diabetes and subsequent foot ulceration. Certain risk factors such as foot deformities, joint issues, and foot perfusion may indicate the risk of developing foot ulcers, according to a study published in the journal Diabetes Care, the flagship publication of the American Diabetes Association (ADA). To carry out the study, researchers examined 749 diabetic veterans and found that patients with hammer/claw toe deformity and a history of laser photocoagulation are at an increased risk of developing foot ulcers. Other risk factors in foot ulcer onset include reduced skin oxygenation and foot perfusion.
Another study published in the same journal suggests that using both neuropathy disability score and vibration perception threshold tests may help identify patients at risk of developing diabetes-related foot ulcers. Foot pressure measurements also how high specificity, and can be used as an alternative post-screening test in patients, researchers say.
A 2009 study revealed that using the Semmes Weinstein monofilament examination (SWME) was an effective way to determine the risk of nerve damage onset in patients. In the study, researchers examined more than 1,000 healthy patients and found that SWME is up to 93 percent sensitive and up to 100 percent specific in identifying patients at risk of diabetes-related nerve damage. These findings appeared in the Journal of Vascular Surgery.
Important points to consider in a foot examination
A report by the ADA’s Task Force of the Foot Care Interest Group highlighted some of the most important components of foot examination.
- Dermatological assessment — This initial step in foot assessment should focus on the presence of possible ulceration, as well as temperature differences between the limbs.
- Musculoskeletal assessment — Take note of any rigid or gross deformity in the foot. These deformities may result in increased plantar pressure, which in turn may trigger the onset of ulceration. It is also important to look out for a condition called Charcot arthropathy, which commonly occurs in midfoot among neuropathic patients.
- Neurological assessment — This assessment helps determine nerve damage in patients. Five simple tests can be used in neurological assessment including 10-g monofilaments score, 128-Hz tuning forks, pinprick sensation test, ankle reflex test, and vibration perception threshold score.
The facts on diabetes
Diabetes remains to be a high-burden disease worldwide that affects as many as 422 million. According to the World Health Organization (WHO), the global prevalence of diabetes has been rapidly increasing since the 1980’s, especially in middle- and low-income countries. The disease leads to a host of adverse complications such as blindness, heart attacks, and lower limb ulceration and amputations.
Foot ulceration and lower limb amputation are some of the most common co-morbid conditions in patients with diabetes. A report by the International Diabetes Federation (IDF) reveals that up to half of all diabetes patients worldwide are at risk of developing foot ulcers. According to the IDF, nerve damage or neuropathy is a key contributor in the onset of diabetic foot ulcers, which affects between 20 to 50 percent of diabetes patients. Neuropathy affects the patients in two ways: it may either trigger painful symptoms in the patients’ legs or induce numbness in the lower limbs. The IDF cautions that while nerve damage does not directly cause injury in patients, the subsequent numbness dampens the foot’s sensitivity to pain and rising temperature. This then renders the patients to be more susceptible to injury without them knowing. Nerve damage is also a major factor in slow wound healing in patients. With slow a slow healing process, foot ulcers may lead to infection over time if not addressed properly.
Increase your lifespan and improve your quality of life by following the articles on Longevity.news.
Sources include:
Tagged Under: diabetes, diabetes detection, diabetic foot ulcer, foot ulcers, nerve damage, nerve pain, prevention